
- IDDSI towards developed standardised terminology for texture modified foods and thickened liquids.
- IDDSI standards were introduced to ensure consistency of texture by creating a series of simple, yet reliable tests for each level of texture modification.
- Drink thickness now has 5 levels, and the food modification level now starts at level 3 and moves up to level 7.
- Understanding the differences in the way food and liquids should be modified is very important – for Chefs, residents, families, and care staff alike.

The International Dysphagia Diet Standardisation Initiative (IDDSI) was introduced in 2020, with a goal to develop standardised terminology for texture modified foods and thickened liquids for people needing different forms of texture modification. The Dieticians Association Australia is one of many international supporters of the standardisation.
Swallowing is a complex function we do both voluntarily and as an automatic reflex. When we eat, food is chewed, moved around in the mouth until it reaches a spot at the back of the tongue where our swallow reflex is triggered. This video animates what happens with dysphagia.

Speech Pathologist, Wendy Forster explains that for residents with Dysphagia, this process is impaired to some degree.
“The brain doesn’t register the normal sensory cues, so eating and drinking becomes a slow and difficult process,” Forster said.
The International Dysphagia Diet Standards have introduced levels of texture modification for liquids and modified texture foods.
The new standards have been introduced to ensure consistency of texture by creating a series of simple, yet reliable tests for each level of texture modification.

Drink thickness now has 5 levels, starting with a grading of 0 for thin, drink textures become gradually thicker up to level 4, extremely thick.
At Level 3 and 4 both food and drink are at the same thickness and require similar testing methods.
1) Mildly Thick:
Fluid runs freely off the spoon but leaves a mild coating on the spoon; the consistency of nectar.
2) Moderately Thick:
Fluid slowly drips in dollops off the end of the spoon; the consistency of gravy.
3) Extremely thick:
Fluid sits on the spoon and does not flow off it; the consistency of custard.
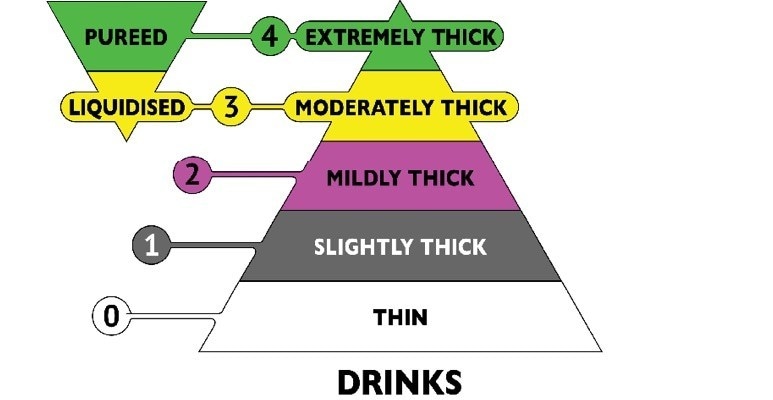
For full instructions on how to create and test for each of the drink levels, refer to the IDDSI resource page.

The food modification level now starts at level 3, liquidised and moves up to level 7, Regular, easy to chew.
1) Soft:
Food may be naturally soft or may be cooked or cut to alter its texture; can be chewed with minimal effort.
2) Minced and Moist:
Food is soft, moist and easily mashed with a fork; lumps are smooth and rounded.
3) Smooth Purée:
Food is smooth, moist and lump free; may have a grainy quality.
A speech pathologist will review the condition and request food be texture modified only to the level the person can safely manage, and no more. Enjoyment of food plays a big role in a person’s enjoyment of life, so losing a favourite food texture is especially hard. If a person enjoyed crispy roasted potatoes, suddenly only being able to eat a smooth puréed potato can be a huge blow, especially if they can still manage a soft texture.
Forster advises that all Aged Care Chefs know and adhere to the current guidelines and understand what they mean for residents. “A person’s level of texture modified food may change over time – upgraded or downgraded – so being aware of the resident’s current status is crucial.”
Forster cautions that assuming everyone needs the same level can become a problem. Over-modifying can be harmful. If the food doesn’t require any chewing it can move too quickly and may not trigger the swallow reflex correctly, even entering the person’s airways causing them to choke. Read more about Wendy Forster’s work with Dysphagia patients here.
Understanding the subtle but important differences in the way food and liquids should be modified is very important – for Chefs, residents, families and care staff alike.
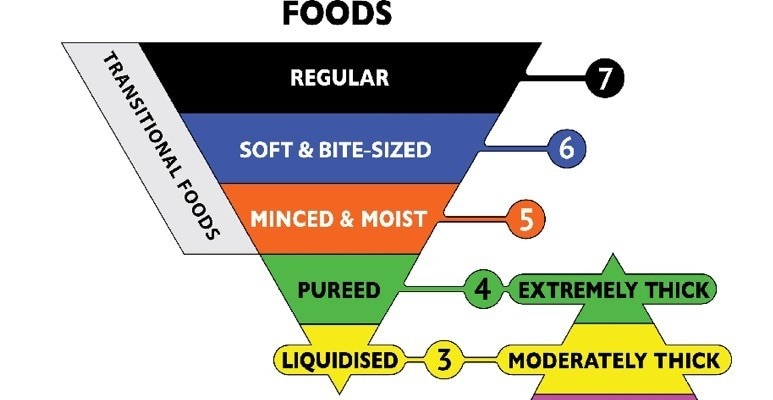
For more information on the new texture levels and testing methods for both drink and food, see our series of IDDSI information articles here.

Disclaimer: The content of this article is created for inspiration purposes only. It is not intended as clinical, medical or nutritional advice.
Top recipes
Related Products
Log in or Create an account to access:
- Get access to this content
- Discover the latest culinary trends
- Explore and save your favourite recipes
- Watch free video training courses for chefs




























